Diabetes-Related Feet and Leg Disease: Early Signs and When to See a Doctor
Diabetes mellitus is a growing concern in Singapore, affecting about one in six adults aged 21 to 69, with lifetime risk projected to reach one in two by 20501. Foot problems are an important cause of morbidity in individuals with diabetes mellitus.
The lifetime risk of foot ulcers in individuals with type 1 or type 2 diabetes may be as high as 34%2, and the worldwide incidence of diabetic foot ulcer is approximately 18.6 million people per year3. Management of diabetic foot ulcers accounts for a large number of hospitalisation stays, has a high rate of readmissions, and is associated with a 2.5-fold risk of death compared with individuals with diabetes without foot ulcers.
In this article, we explain what diabetes-related foot complications are, the early signs and symptoms to watch for, and why these changes occur. We also cover practical steps for prevention, including daily foot care, proper footwear, and blood sugar management, along with when to seek medical attention to reduce the risk of complications.
What Is Diabetes-Related Feet Disease?
Diabetes-related foot disease, or “diabetic foot disease”, is a broad term used to describe foot problems linked to diabetes:
- Peripheral neuropathy: Reduced sensation in the feet
- Charcot foot: Weakening of the bones and joints in the foot
- Peripheral artery disease: Reduced blood flow to the feet
- Foot ulcers or wounds: Open sores or injuries on the feet
- Infection: Bacterial or fungal infection of the foot tissues
- Gangrene: Death of tissue due to lack of blood supply or severe infection
- Amputation risk: Loss of limb in advanced cases
Early signs of diabetes-related foot disease refer to the initial stage of foot complications caused by diabetes mellitus. At this stage, subtle changes begin to occur due to prolonged high blood sugar levels.
It typically involves early nerve damage (known as diabetic neuropathy) and reduced blood circulation in the feet. These changes may not seem serious at first, but they can progress if left unmanaged. Early detection of diabetic foot symptoms is crucial, as this can help prevent severe complications such as infections, ulcers, or even amputation.
What Causes Early Signs of Diabetes-Related Feet Disease?
High blood glucose levels over time can damage both nerves and blood vessels in the body, especially in the feet. Nerve damage (peripheral neuropathy) affects the ability to feel pain, heat, or injury, while blood vessel damage (peripheral artery disease) reduces blood flow, affecting the foot’s ability to heal properly.
As a result, individuals may experience reduced sensation and slower wound healing, resulting in foot ulcers or wounds, infections, and, in severe cases, gangrene. Many symptoms stem from complications of minor injuries that go unnoticed and worsen over time.
Early Signs of Diabetes-Related Feet Disease to Watch For
Recognising early symptoms can make a significant difference in preventing complications. These symptoms generally fall into three categories:
Nerve Symptoms
Early nerve damage, or peripheral neuropathy, can present in several ways:
- Tingling sensations: Often described as “pins and needles,” this is one of the earliest warning signs
- Numbness: Loss of protective sensation makes it risky to walk barefoot, as injuries may go unnoticed
- Burning or sharp pain: These symptoms are often worse at night
- Itchiness: Nerve damage can sometimes cause unexplained itching in the feet
Charcot Foot
Charcot foot is a serious condition in which the bones and joints of the foot become weakened and damaged, typically in the presence of peripheral neuropathy. In the early stages, the foot may appear red, swollen, and warm. As the condition progresses, the foot may change shape or even collapse.
Some patients experience little or no pain despite significant damage, so early signs of Charcot foot are often overlooked. Any swelling, warmth, or change in the shape of the foot should therefore be assessed promptly.
Foot Deformities and Pressure Points
Foot problems can present in several ways, including structural deformities, abnormal pressure points, and changes in the shape or alignment of the foot.
- Claw or hammer toes: Abnormal bending of the toe joints
- Bunions: A bony bump at the base of the big toe
- Prominent pressure points: Areas of increased pressure on the foot
- Flat or high arches: Abnormal arch shape of the foot
Mild deformities may lead to increased pressure in certain areas. Over time, this may lead to thickened skin, calluses, and eventually wounds.
Circulation Signs
Reduced blood flow can lead to visible and physical changes in the feet:
- Colour changes: Skin may appear pale, bluish, or reddish
- Cool feet: A noticeable drop in temperature compared to the rest of the body
- Slow-healing wounds: Cuts or blisters take longer than usual to heal
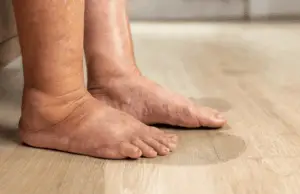
- Swelling (oedema): Fluid buildup in the feet or ankles, sometimes linked to poor circulation or high blood sugar
In more severe cases, this may lead to pain at rest, non-healing wounds, blackened skin or toes, and tissue loss.
Skin and Nail Changes
Skin and nail health can also be affected in early diabetic foot:
- Dry, cracked skin: Reduced sweating from nerve damage leads to dryness, increasing the risk of skin breakdown
- Thickened or discoloured nails: Often caused by fungal infections
- Increased infection risk: Even small cracks or cuts can become infected (including fungal infections like Candida), often accompanied by itchiness
Certain skin conditions are also more common in people with diabetes:
- Necrobiosis lipoidica: Reddish-brown patches, usually on the lower legs
- Diabetic dermopathy: Light brown, scaly patches often found on the shins
When Should You See a Doctor for Diabetic Foot Symptoms?
It is important to seek medical attention early if you notice any changes in your feet. Prompt treatment can prevent minor issues from becoming serious complications.
You should see a doctor if you experience:
- Wounds or sores that fail to heal
- Signs of infection, such as redness, warmth, swelling, discharge, or an unpleasant smell
- New onset of numbness, tingling, or pain
You should also seek medical advice if you notice any of the following symptoms:
- Ongoing tingling, burning, itching, or discomfort in the feet
- Changes in skin colour
- Dry or cracked skin on the feet that doesn’t improve
- Reduced sensitivity to heat, cold, or pain
- Thickened, discoloured (yellow) toenails
- Hair loss on the toes, feet, or lower legs
- Fungal infections, such as athlete’s foot between the toes
- Ingrown toenails, blisters, ulcers, or infected corns
- Blackened skin or toes
- Swollen or warm foot with little pain
- Sudden change in foot shape
Addressing any warning symptoms with your doctor or endocrinologist promptly can prevent complications such as infections, ulcers, and long-term damage.
Risks of Ignoring Early Signs of Diabetes-Related Feet Disease
Ignoring early symptoms of diabetic foot can lead to serious health consequences. One of the main concerns is diabetic neuropathy, which reduces the ability to feel pain. This means injuries may go unnoticed and untreated.
Without proper care, diabetic foot problems can progressively worsen, leading to:
- Diabetic foot ulcers: Open sores that are difficult to heal
- Infections: Bacterial or fungal infections that can spread quickly
- Tissue damage: Including skin and deeper structures
In severe cases, untreated infections and tissue damage may necessitate amputation to prevent the spread of infection.
Treatment For Diabetes-Related Feet Disease Complications
There are several treatment approaches available for managing early diabetic foot complications. These treatments focus on promoting healing, preventing infection, and addressing underlying issues such as diabetic neuropathy and poor circulation to reduce the risk of progression.
Wound Management
Initial treatment focuses on proper wound care to promote healing and prevent infection.
Basic wound care includes:
- Cleaning the wound: Removing dirt, debris, and bacteria
- Draining fluid or pus: If infection is present
- Debridement: Removal of dead or infected tissue to support healing
Healthcare providers may also use:
- Specialised dressings and ointments: To keep the wound moist and absorb excess fluid
- Offloading pressure: Using appropriate footwear, braces, or mobility aids to reduce stress on the affected area
For mild infections, oral antibiotics may be prescribed.
Advanced Treatment
More severe cases require intensive medical care. Treatment options may include:
- Intravenous antibiotics: For serious or spreading infections
- Hospitalisation: For close monitoring and comprehensive treatment
- Surgical debridement: To remove extensive dead or infected tissue
In advanced situations, surgery may be necessary to control infection and prevent further complications. In the most severe cases, amputation may be required to stop the spread of infection. As such, prompt treatment significantly reduces the likelihood of these major interventions.
How to Prevent Diabetes-Related Feet Disease Complications
Preventive care is essential in reducing the risk of diabetic foot problems. Simple daily habits can go a long way in protecting your feet, especially since diabetes can affect both sensation and healing.
Maintain Proper Foot Hygiene
Keeping your feet clean helps prevent infections and allows early detection of any changes.
- For daily cleansing: Wash your feet with lukewarm water and mild soap to remove dirt and bacteria. Avoid hot water, as reduced sensation from diabetic peripheral neuropathy may prevent you from detecting excessive heat.
- Thoroughly dry your feet: Dry your feet after washing, especially between the toes, as excess moisture can encourage fungal infections.
Care for Diabetic Foot Skin
Proper skin care is essential because diabetes often leads to dry, fragile skin, which can crack easily and increase the risk of infection if not properly managed.
- Hydrate your skin daily: Apply moisturiser to keep your skin soft and prevent dryness and cracking.
- Apply moisturiser correctly: Focus on the tops and soles of your feet while avoiding the spaces between the toes, as they are more susceptible to fungal growth.
- Check your skin regularly: Identify dry, cracked, or peeling areas early to prevent infection.
Practice Safe Nail Care
Practising safe and careful nail care is important in preventing injuries such as cuts or ingrown toenails, which can become serious if left untreated.
- Trim your nails properly: Cut your toenails straight across to prevent ingrown nails.
- Smooth rough edges: Use a nail file to gently remove sharp corners that could snag on surrounding fabric and injure your nail.
- Avoid cutting nails too short: This protects the surrounding skin from injury and infection.
- Seek professional care when needed: Consult a healthcare provider if your nails are thickened, discoloured, or difficult to manage.
Choose Appropriate Footwear
Wearing appropriate footwear plays a key role in protecting your feet from pressure, friction, and accidental injury, all of which can lead to complications in people with diabetes.
- Choose well-fitting shoes: Ensure a comfortable fit with cushioned soles and a wide toe box to prevent crowding
- Select breathable materials: This reduces moisture and sweat buildup inside your shoes.
- Inspect your shoes regularly: Check for rough edges, damage, or foreign objects before wearing them.
Perform Daily Diabetic Foot Inspection
Performing daily foot inspections is crucial because reduced sensation means injuries can easily go unnoticed until they become more serious.
Check your feet every day using a mirror to see all areas, including the soles, heels, sides, and between the toes. While inspecting your feet, look for early signs of diabetic foot such as cuts, blisters, redness, swelling, or colour changes.
Maintain Blood Sugar Control
Keeping blood sugar and HbA1c levels healthy is one of the most effective ways to prevent diabetic foot complications, as they directly impact both nerve health and blood circulation. By keeping blood sugar levels within target range, you can prevent damage to nerves and blood vessels, lowering the likelihood of developing conditions such as diabetic neuropathy.
Using an insulin pump can be an effective tool to help manage blood sugar levels more consistently. An insulin pump delivers a steady, controlled dose of insulin, which can help maintain tighter blood sugar control and prevent the fluctuations that might otherwise increase the risk of complications like neuropathy.
If you have diabetes and are unsure how to better manage your blood sugar levels, consult an endocrinologist for personalised guidance and treatment options.
FAQs About Diabetes-Related Feet Disease
Why are people with diabetes more likely to develop foot problems?
Diabetes can affect both the nerves and the blood vessels. Nerve damage may reduce sensation in the feet, making it harder to notice injuries early. At the same time, reduced blood flow can slow healing and increase the risk of complications.
Can I have a serious foot problem even if I do not feel pain?
Yes. People with diabetic peripheral neuropathy may have little or no pain even when significant problems such as calluses, ulcers, deformities, or deep infections are present. Regular foot checks are important, even when the feet feel normal.
What are the early signs of diabetic foot disease?
Early signs may include numbness, tingling, or burning sensations, as well as dry or cracked skin. Other warning signs include changes in skin colour or temperature, swelling, calluses, thickened nails, new blisters, or sores that are slow to heal.
What is a diabetic foot ulcer?
A diabetic ulcer is an open sore or wound that develops as a complication of diabetes. It is typically caused by a combination of poor blood circulation and nerve damage, both of which can result from prolonged high blood glucose levels.
These ulcers most commonly appear on the feet or lower legs. Because diabetes can reduce sensation, individuals may not notice minor injuries such as cuts or pressure points. At the same time, reduced blood flow slows the body’s natural healing process, allowing wounds to worsen and potentially become chronic.
Does every foot problem in diabetes mean amputation?
No, not every foot problem leads to amputation. However, some conditions can become serious if treatment is delayed, particularly when infection, severe deformity, neuropathy, or poor circulation are present.
Amputation may be necessary in severe cases where the foot or leg is damaged beyond recovery. Nerve damage (peripheral neuropathy) can reduce sensation, allowing injuries to go unnoticed and worsen. In addition, poor circulation (peripheral artery disease) can delay wound healing.
If wounds become infected and progress to gangrene, amputation may be required to prevent the spread of infection. This makes early assessment and treatment important.
What does poor circulation in the feet look like?
Poor circulation may present as slow-healing wounds, changes in skin colour, cooler skin, pain in the legs when walking, or pain at rest. In more severe cases, blackened areas of skin may develop. Reduced blood flow can make healing more difficult and increase the risk of serious complications.
When should I see a doctor for diabetic foot disease?
You should seek medical attention if you notice numbness, tingling, a blister, a cut, redness, swelling, warmth and a non-healing wound, a change in foot shape, a fungal infection or any colour change in the foot. Daily self-checks are important so problems can be picked up early.
Urgent review is important if there is pus, a foul smell, spreading redness, fever, blackened skin, sudden swelling with deformity, or a wound that appears deep. These can be signs of a more severe infection or reduced blood flow.
Can diabetic foot problems be prevented?
Many serious foot problems can be reduced with regular care. This includes daily foot checks, wearing well-fitting footwear, maintaining good skin care, and managing blood glucose and cardiovascular risk factors. Early review of any changes in the feet is essential.
If you have diabetes and are concerned about your risk of diabetic-related foot disease, schedule a consultation with Dr Linsey Gani for personalised advice on how you can better manage this condition.
Disclaimer
This information is provided for general education. It does not replace personalised medical advice. Please consult your doctor for guidance on the medications that may be appropriate for you.
1Retrieved from SingHealth
2Retrieved from The New England Journal of Medicine
3Retrieved from PubMed

Dr Linsey Gani is an endocrinologist experienced in conditions related to hormonal imbalances, including those affecting fertility, menstrual health, and reproductive function. Dr Gani completed her residency in Melbourne, Australia. She is a fellow of the Royal Australian College of physician and the Academy of Medicine, Singapore.
Related Articles

Gestational Diabetes Mellitus (GDM) in Singapore: Symptoms, Causes, and Management
Gestational Diabetes Mellitus (GDM) in Singapore: Symptoms, Causes, and Management Gestational diabetes mellitus (GDM), also known as pregnancy-induced diabetes, is

Adiposity-Based Chronic Disease (ABCD): A Modern Medical Approach to Excess Body Fat
Adiposity-Based Chronic Disease (ABCD): A Modern Medical Approach to Excess Body Fat Obesity is often misunderstood and linked to personal

Insulin Pump Singapore: How It Works, Who Should Use It, and Costs
Insulin Pump Singapore: How It Works, Who Should Use It, and Costs Diabetes is common in Singapore, with 9.1% of
